Sport
Lo sport va a cercare la paura per dominarla, la fatica per trionfarne, la difficoltà per vincerla.
– Pierre de Coubertin –
Introduzione
Gli atleti non sono pazienti comuni, sia per l’eccezionalità delle prestazioni che esprimono tutte le volte che praticano il proprio sport, sia perché quando sono vittime di traumi ne possono risentire, non solo fisicamente, come tutti noi, ma anche umanamente e professionalmente.
Tuttavia, c’è da constatare che a volte basterebbe osservare il suggerimento del riposo per ridurre o risolvere i problemi che spesso li portano a doversi affidare alle cure di un ortopedico.
Quando un paziente così speciale arriva da me di solito è perché ha una stringente necessità di ridurre i tempi di recupero o di spostare un po’ più in là l’asticella dei propri limiti fisici.
Per aiutarlo in questa impresa, apparentemente sovrumana, io mi ispiro innanzitutto al principio incontrovertibile dei Padri della medicina (“Primum non nocere”), in secondo luogo all’innovazione e, inoltre, ad un costante lavoro di formazione ed aggiornamento professionale.
Così aiuto i miei pazienti “speciali” a spostare un po’ più in là i propri limiti, nel rispetto tanto della legge, quanto dell’etica professionale ovviamente.
Per sintetizzare la vastità di problematiche fisiche che possono popolare l’universo di uno sportivo riporto di seguito alcune parole chiave nella casistica delle patologie sportive ma innanzitutto qualche consiglio di buonsenso su come prevenire certi traumi.
Torna in cimaProsegui
Prevenzione


Quando si parla di piede e caviglia, prevenire vuol dire innanzitutto scegliere una calzatura adeguata alle proprie esigenze, ma anche studiare l’appoggio del piede sia da fermo che in movimento.
Chiunque si sia affacciato negli ultimi anni alla pratica dell’ormai popolarissima maratona o running (ma vale anche per il fondo o mezzofondo in atletica), si sarà reso conto navigando su internet di quanti siti, più o meno blasonati, si affrettino a dare consigli sulla scelta della scarpa più adeguata, in funzione di quella che può essere la conformazione del proprio piede: pronatore, supinatore o neutro.
Lo stesso vale per i tanti negozi specializzati in abbigliamento e attrezzature sportive che vedono spesso tanto solerti quanto sprovveduti commessi ergersi a specialisti dell’ortopedia umana.
Per consigliare efficacemente uno specifico tipo di scarpa (da pronatore o da supinatore per esempio) è necessario aver studiato e compreso l’intero ciclo del passo e valutare i rischi di sovraccarico che possono sopraggiungere nel compiere un determinato gesto tecnico.
Persino un’analisi computerizzata del passo può risultare inutile, se non associata ad un’attenta valutazione clinica.
Effettuare una scelta corretta vuol dire ridurre i rischi di sovraccarico e soprattutto le patologie da “over use” dell’atleta: tendiniti, borsiti, ma anche fratture da stress e microfratture.
Compiere una scelta sbagliata vuol dire, alla lunga, indurre una patologia.
A titolo del tutto esemplificativo possiamo citare la recente “class action” promossa in USA, dagli utilizzatori di scarpe minimaliste contro le aziende produttrici.
Attribuire a priori la colpa del danno fisico all’uso di scarpe minimaliste da running non è corretto. Tuttavia, utilizzarle indiscriminatamente senza valutare i rischi o i vantaggi per l’atleta che le utilizza, può sicuramente rappresentare un problema.
Per questo considero fondamentale effettuare una valutazione clinica del paziente e dell’atleta, talvolta associandola a esami strumentali funzionali (baropodometria) e/o di imaging (Rx in carico) e all’accurato studio del gesto tecnico sportivo.
Per completare al meglio la valutazione, consiglio di presentarsi alla visita con una descrizione dettagliata del piano di allenamenti e con una ripresa video dell’abituale performance dell’atleta.
A tal proposito ho recentemente condotto e pubblicato, in collaborazione con il Politecnico di Milano e l’Università di Liverpool, uno studio sulla scarpa da rugby, e sulle diverse sollecitazioni a cui è sottoposto il piede di un giocatore in funzione del ruolo ricoperto in campo.
Ovviamente, le calzature per quanto all’avanguardia restano sempre prodotti di serie e possono non essere sufficienti a soddisfare le peculiari esigenze di ciascun atleta.
Per questo possono risultare utili i plantari, da non intendersi come un semplice sostegno della volta plantare, ma come speciali strumenti da studiare e progettare – caso per caso – in funzione dello specifico e del tutto personale gesto tecnico dell’atleta.
Per concludere, c’è da osservare che anche le forze di taglio (ossia gli attriti) possono rappresentare un importante fattore usurante.
Per questo, oggi sono stati pensati dei semplici plantari neutri e molto sottili, che non hanno alcuna funzione di compenso biomeccanico, se non quella di ridurre gli attriti.
Anche in questo caso, un uso indiscriminato di questi supporti, non solo può essere inutile ma anche dannoso, quindi è sempre necessario affidarsi a persone competenti e titolate a suggerirne l’impiego.
Torna in cimaProsegui
I muscoli e i tendini
Il muscolo, per la capacità contrattile e il tendine, per la sua capacità elastica, possono andare incontro a rottura/lesione (strappo e stiramento) o a patologie da sovraccarico (tendinosi e tendiniti).
Lesioni acute (strappo/stiramento)
Quando si è in presenza di questo tipo di lesioni è sbagliato pensare che immobilizzazione e riposo portino da sole alla guarigione in tempi soddisfacenti.
È invece importante, qualora sussista il ragionevole dubbio di essere in presenza di una di lesione muscolare o miotendinea, eseguire una pronta diagnosi, grazie ad una semplice ecografia, per ottenere informazioni sulla sede della lesione e sull’entità della lesione stessa.
Accertata la lesione muscolare, esiste davvero poco o nessuno spazio per la chirurgia; tuttavia, la biologia oggi è di grande in aiuto.
Infatti, è possibile utilizzare i PRP (o fattori della crescita) per stimolare processi di auto-guarigione.
L’abbinamento poi di un piano che preveda il corretto impiego di terapie fisiche innovative (Tecar Terapia, Interx, Cheltherapy) può fare la differenza nel garantire un recupero veloce e nel ridurre eventuali postumi.
Nel caso di lesione tendinea acuta, può essere necessario ricorrere alla chirurgia, stando ben attenti però a conciliare due importanti aspetti:
- ridotta invasività;
- stabilità della riparazione.
Ancora una volta i PRP renderanno tutto estremamente più veloce.
Lesioni croniche o acute (tendiniti, tendinosi, fibrosi, tendinopatie)
Le lesioni croniche possono essere esito di una lesione acuta che generi cicatrici e fibrosi o che semplicemente si cronicizzi.
Ulteriore causa di una lesione cronica può essere uno scorretto gesto tecnico o una non corretta scelta della calzatura. In questi casi è la prevenzione che è venuta meno ed è su quella che si dovrà lavorare.
Ovviamente anche in questo caso, come già anticipato per le lesioni acute, i PRP e le cellule multipotenti prelevate dal tessuto adiposo fanno la differenza in termini di tempi di recupero ed efficacia.
A completare il set di frecce all’arco di un buon ortopedico che si faccia carico della delicata cura di un’atleta ci sono poi tutte le terapie fisiche innovative (Tecar Terapia, Interx e Cheltherapy), associate a tecniche di fisioterapia moderne (fibrolisi, pompage, osteopatia, chiropratica, kinesiotaping).
Compito delicato per il medico sarà di personalizzare, di caso in caso, l’iter terapeutico, dettando i tempi.
Torna in cimaProsegui
I legamenti: l’instabilità di caviglia e del piede


Caviglia
I tanto noti “traumi distorsivi della caviglia” possono portare a lesioni legamentose, che non sempre sono di interesse chirurgico.
Si tratta di traumi che possono interessare in particolar modo giocatori di basket e pallavolo, calciatori e rugbisty, ma anche persone comuni, con o senza l’abitudine ad una regolare attività fisica.
I legamenti della caviglia, al contrario di quelli del ginocchio, sono per lo più extra articolari.
Per capire meglio:
nel ginocchio i legamenti sono come i raggi della ruota di una bici, cioè intra-articolari e contribuiscono in maniera fondamentale alla stabilità della struttura. Nella caviglia questi raggi si trovano al di fuori della struttura. Ne consegue una maggiore esposizione alle lesioni ma al tempo stesso un minore impatto sulla stabilità della caviglia.
Mi capita spesso di ricevere in studio pazienti preoccupati per l’esito di una risonanza che descrive legamenti completamente lesionati. In realtà, come spiego loro, i legamenti della caviglia si lesionano assai più facilmente che quelli di altre articolazioni, ma ancora più spesso guariscono in seguito ad una fibrosi cicatriziale che restituisce all’articolazione l’originaria stabilità dei legamenti.
Risulta fondamentale, anche in questo caso, la rieducazione mediante terapie fisiche e fisioterapia (Tecar Terapia, kinesiotaping, fisiokinesiterapia) per recuperare articolarità.
E successivamente la rieducazione propriocettiva, per abituare la caviglia ai cambi di direzione, alle asperità del terreno, usando apposite tavolette ed esercizi pensati su misura per il paziente.
Solo nel 15-20% dei casi una lesione legamentosa determina instabilità cronica, ossia la tendenza della caviglia a cedere.
È in questa situazione che è invece necessario intervenire chirurgicamente. Si tratta di interventi eseguiti ormai con tecniche mini-invasive, non solo con l’obiettivo di ridare stabilità alla caviglia, ma anche di prevenire eventuali recidive di traumi distorsivi e concomitanti lesioni della cartilagine.
Piede
I traumi distorsivi possono anche interessare la regione del mesopiede, determinando i cosiddetti traumi della Lisfranc, dal nome di uno dei medici di campo di Napoleone, che definì una tecnica per eseguire l’amputazione di piedi gravemente lesionati dei soldati feriti lungo una ben precisa area dello stesso: quella che congiunge il mesopiede ed il retropiede.
Lasciando da parte i pur valorosi soldati napoleonici, i guerrieri dei nostri tempi che più di altri incorrono in lesioni in quest’area del piede sono i giocatori di rugby e football americano.
Gli spettacolari quanto pericolosi tuffi in corsa di un difensore sul piede di un avversario lanciato a meta sono generalmente la principale causa di queste lesioni.
Paradossalmente questo tipo di lesioni accomuna ai rugbisty una categoria di atlete di tutt’altra tempra e con una decisamente più spiccata grazia: le ballerine.
La posizione “en-pointe” (un modo di vivere quotidiano per queste artiste) può determinare lesioni legamentose, ma anche ossee, da stress proprio a livello di questa regione anatomica.
Si tratta di lesioni con un decorso molto più lento e insidioso dei traumi distorsivi della caviglia che possono richiedere con maggior frequenza un intervento di stabilizzazione, come spiego in uno studio che ho pubblicato nel mio periodo di lavoro presso la Duke University (Lisfranc injuries in sport).
Torna in cimaProsegui
L’impingement postero-mediale del flessore lungo dell’alluce nella ballerina


Si tratta di una vera e propria patologia professionale. Curare quello che è il fulcro esistenziale di queste eccezionali danzatrici è per un chirurgo con la mia specializzazione una sfida terapeutica ardua ma al tempo stesso gratificante.
È un po’ come per i miei colleghi, focalizzati sulla mano, prendersi cura di un pianista o di un violinista.
Nella danza classica la sollecitazione della calzatura e della posizione “en-pointe” può determinare un’alterazione anatomica a livello dell’astragalo (l’osso del retropiede che si articola con la caviglia).
Questa alterazione anatomica consiste in un ispessimento fibroso del margine postero-mediale dell’astragalo che porta ad un conflitto (ossia ad irritarlo nel suo scorrimento) con il tendine flessore lungo dell’alluce.
La paziente di solito lamenta difficoltà a tenere la posizione “en-pointe”, crampi al polpaccio e dolore all’interno della caviglia, esacerbato dalla flessione dell’alluce.
All’inizio si può cercare una soluzione non invasiva raccomandando riposo e prescrivendo un’adeguata terapia fisica (Tecar Terapia).
Qualora la strada conservativa si dimostri insufficiente o inefficace si passerà a quella chirurgica.
In questi casi è necessario ricorrere ad una lisi postero-mediale con asportazione della causa del conflitto (os trigonum) e dell’ispessimento fibroso.
Nella maggior parte dei casi questo intervento è eseguibile in artroscopia, tecnica che consente di ridurre al minimo l’invasività (richiede portali artroscopici posteriori) e soprattutto i tempi di recupero.
Resta comunque da valutare, per ogni singolo caso, la possibilità di scegliere questa tecnica in luogo di quella più tradizionale per poi stabilire i tempi per il ritorno sul palcoscenico.
Torna in cimaProsegui
Le ossa: fratture da stress
La frattura di un osso non sempre è conseguente ad un trauma acuto. Infatti, piccoli ma continui e ripetuti traumi possono determinare fratture da stress.
Gli atleti più esposti a questi rischi sono senza dubbio i maratoneti.
Le tipiche fratture da stress in cui incorrono più frequentemente questi sportivi interessano i metatarsali e sono favorite da una particolare lunghezza di questi ultimi (nel caso del secondo e del terzo) o da un piede cavo (nel caso del quinto metatarsale).
Raramente è necessario intervenire chirurgicamente per sanare questi problemi. Molto più efficaci risulteranno adeguate terapie fisiche e l’utilizzo dei fattori di crescita (PRP e cellule stromali multipotenti del grasso).
Tutto ciò ovviamente deve essere guidato e supervisionato da un esperto chirurgo del piede che sappia, non solo tracciare il più corretto iter terapeutico, ma sia anche in grado di valutare accuratamente il gesto tecnico dell’atleta e suggerire l’uso di una calzatura adatta che riduca il rischio di recidiva del problema.
Un altro osso comunemente soggetto a fratture da stress è lo scafoide.
In questi casi, scelte chirurgiche mini-invasive di sintesi percutanea si dimostrano spesso più soddisfacenti di approcci chirurgici classici, favorendo inoltre tempi di guarigione rapidi.
Vale anche in questo caso la raccomandazione sulla scelta di un professionista specializzato.
Per concludere cito le ballerine quali soggetti altamente esposti al rischio di frattura da stress, a livello della base del secondo metatarsale; ancora una volta la causa scatenante è la posizione “en-pointe”.
Torna in cimaProsegui
PRP e cellule multipotenti della frazione stromale del tessuto adiposo
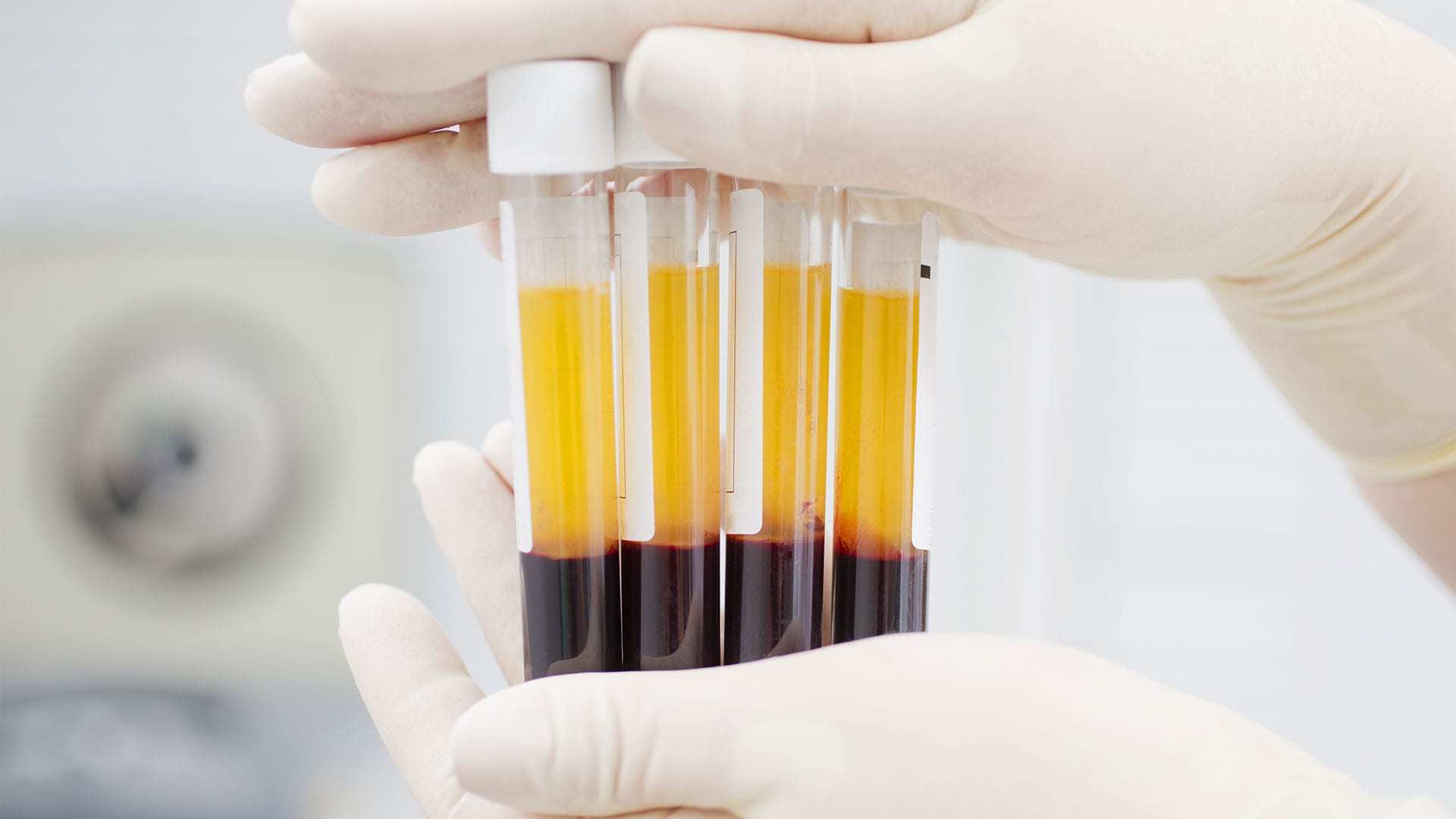

Più volte sono state citate nella disamina fatta sopra e per questo è opportuno descrivere brevemente, le sorprendenti capacità rigenerative delle PRP e delle cellule multipotenti.
Nel nostro sangue esistono dei fattori di crescita di derivazione piastrinica in grado di indurre riparazione e rigenerazione tessutale.
Basta un semplice prelievo del sangue del paziente, sottoporlo a centrifugazione e procedere quindi all’estrazione dei fattori di crescita.
Compiuta questa operazione si effettua, con una semplice iniezione, il reinserimento nell’organismo umano dei fattori nella zona anatomica malata.
Ovviamente non si tratta di una panacea da cui aspettarsi guarigioni miracolose, ma è sicuramente uno strumento in più a disposizione di medici esperti e responsabili che possono utilizzarlo a beneficio di più efficaci e veloci cure, sia per gli sportivi che per tutti gli altri pazienti.
È recentissima poi la scoperta dell’enorme potere rigenerativo che hanno le cosiddette cellule multipotenti della frazione stromale del tessuto adiposo che si trovano appunto nel tessuto adiposo umano (il grasso).
Una volta prelevate dall’area di origine possono differenziarsi e dare vita a fenomeni proliferativi e riparativi del tessuto nel quale vengono successivamente iniettate e ospitate.
La maggiore efficacia ipotizzata è legata al fatto che i PRP veicolano dei messaggeri di rigenerazione per le cellule locali, le cellule stromali multipotenti arricchirebbero il patrimonio cellulare locale, oltre a portare i messaggeri di rigenerazione.
Il prelievo viene eseguito in anestesia locale. Con un particolare ago si procede all’aspirazione di una piccola quantità di tessuto adiposo che poi viene filtrato per isolare le cellule stromali multipotenti; queste saranno poi iniettate nella zona malata da trattare.
Evidentemente questi due processi sono molto simili fra loro e al momento non esiste un’evidenza scientifica a favore dell’uno o dell’altro. Sono entrambe procedure sicure, con un grande potenziale terapeutico.
Attualmente sono responsabile di uno studio scientifico prospettico sostenuto da IRCCS Galeazzi dove ho lavorato 10 anni prima del passaggio in Humanitas San Pio X come responsabile di Ortopedia della Caviglia e del Piede che, per la prima volta, confronta l’efficacia delle due metodiche nella patologia del tendine d’Achille.
I risultati preliminari sono incoraggianti.
Torna in cimaScrivimi